Study Points
- Back to Course Home
- Participation Instructions
- Review the course material online or in print.
- Complete the course evaluation.
- Review your Transcript to view and print your Certificate of Completion. Your date of completion will be the date (Pacific Time) the course was electronically submitted for credit, with no exceptions. Partial credit is not available.
Study Points
Click on any objective to view test questions.
- Articulate the history and burden of influenza on the community.
- Explain the types of influenza viruses, including the H and N designations.
- Describe the symptoms, transmission, and diagnosis of influenza.
- Distinguish between influenza and influenza-like illnesses.
- Identify complications of influenza.
- Articulate the effectiveness and importance of the influenza vaccines.
- Implement a strategy to increase vaccine administration to vulnerable patients.
- Describe the best method of hand hygiene and other ways of protecting against influenza.
- List the current antiviral medications available and their use.
- Teach family members how to care for people with the flu, including interventions for non-English-proficient patients and caregivers.
- Identify the significance of avian and swine influenza, particularly issues related to pandemic disease.
During the 2009 H1N1 pandemic, what percentage of hospitalizations and deaths were in persons younger than 65 years of age?
Click to ReviewRates of serious illness and death from seasonal influenza are higher among those who are 65 years of age and older [3]. During the 2023–2024 flu season, the hospitalization rate in this age group was 400.5% (per 100,000 population) compared with 153.4% in adults 50 to 64 years of age and 65.4% in those 18 to 49 years of age. The mortality rate was also higher at 32.1% compared with 9.1% in those 50 to 64 years of age and 1.9% in those 18 to 49 years of age [3]. Pediatric deaths increased from 427 during the 2022–2023 flu season to 521 during the 2023–2024 influenza season [3]. During flu pandemics, the burden of disease has skewed toward younger individuals; in the 2009 H1N1 pandemic, which caused illness in 60 million Americans, 90% of hospitalizations and deaths were in persons younger than 65 years of age [4].
For many years, the proposed influenza epicenter was thought to be
Click to ReviewFor many years, the proposed influenza epicenter has been thought to be Southeast Asia. Farming practices there bring pigs, fowl, and people into close contact, allowing swine, avian, and human flu viruses to mix. The cycle is thought to be birds to pigs to humans. Now it is clear that this cycle can occur at any place in the world where there is the domestication of animals [12].
In humans, the type of flu that usually causes the most severe illness in humans is influenza type
Click to ReviewInfluenza type A is the virus that causes moderate-to-severe illness in all age groups and is highly infectious, with an attack rate of 10% to 20%. It also causes influenza in pigs, birds, and other animals. There are several subtypes of influenza A.
Antigenic shift means
Click to ReviewThe genes of influenza viruses are carried on eight separate segments of RNA rather than on one long single molecule. This means that if two or more subtypes of influenza virus infect the same cell in a host, these viruses can exchange RNA segments during replication and create viruses with new gene combinations. This reassortment is termed "antigenic shift." It often occurs in pigs and is the source of influenza epidemics because the human population has little immunity to the new subtype that results.
Antigenic drift means
Click to ReviewIn comparison, "antigenic drift" refers to changes in the surface glycoproteins. This does not result in a new subtype but does influence the choice of the particular influenza viral subtypes for the annual influenza vaccine. Depending on the degree of antigenic drift, immunity developed to one virus may be adequate to protect against the related virus. In other situations, the drift has resulted in enough change that there is little protection.
The major symptoms of influenza are
Click to ReviewAs noted, before the emergence of COVID-19, it was relatively easy to diagnose influenza. This is no longer the case, as the viral infections cause similar symptoms [14]. Uncomplicated influenza (and COVID-19) is characterized by an abrupt onset of:
Constitutional symptoms: Fever, chills, myalgia, headache, severe and persistent malaise, eye pain, light sensitivity, and substernal burning in the chest
Respiratory symptoms: Nonproductive cough, shortness of breath, sore throat, and rhinitis
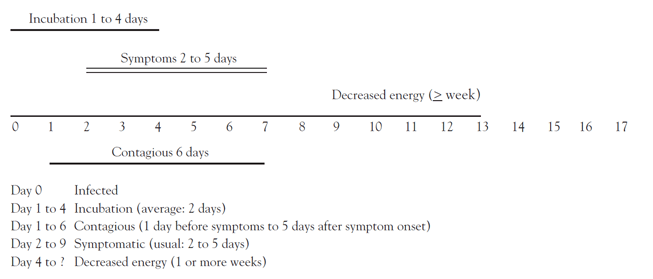
The incubation period of influenza in adults is usually
Influenza is transmitted to other people by
Click to ReviewInfluenza is highly contagious, with an attack rate of 10% to 20% from the day before symptoms begin through approximately five days after onset in adults. It is spread from person to person through coughing and sneezing by the infected individual. Influenza is spread by the airborne route, which means that a person coughing in the room can transmit the virus to others in the room without close personal contact. This is in contrast to droplet transmission in which heavier particles (droplets) are transmitted to those with close contact (less than 3–6 feet, depending on the organism). Droplet transmission also probably occurs in influenza. Airborne transmission is especially significant in congregate situations like institutions, daycare facilities, airplanes, and cruise ships [17].
Rapid tests for influenza are
Click to ReviewObviously, an accurate diagnosis of influenza on the basis of symptoms alone is difficult. The quickest way to decide if the patient has influenza, COVID-19, or some other disease, is to use rapid diagnostic tests for influenza and COVID-19. However, medical practitioners should be aware that false-negative and false-positive results do occur. All patients with flu-like symptoms should now be administered rapid diagnostic tests to identify influenza and/or COVID-19 infection(s) [14].
One disease that could be misdiagnosed as influenza is
Click to ReviewBecause both influenza and the common cold are caused by viruses that affect the respiratory tract, distinguishing between them is important. Adults rarely develop fever with a cold (coryza) but usually have a fever of 101 to 102 degrees F (38.3 to 39 degrees C) with the flu. Headaches, muscle aches, and extreme exhaustion are mild or nonexistent with a cold but are usual and severe with the flu. The prodromal signs of sneezing, runny nose, and sore throat signal that a cold is developing and may be present for one or more days before onset. These symptoms may occur with influenza but usually occur concurrently with the sudden onset rather than signaling an approaching illness. The flu develops suddenly, without warning. Like influenza, a cold may have a dry (nonproductive) cough. Some use a simple rule to distinguish between a cold, in which symptoms are from the neck up, and influenza, which is systemic (Table 1).
Which of the following is a characteristic of influenza but not the common cold?
Click to ReviewINFLUENZA COMPARED TO COMMON COLD
Clinical Presentation Influenza Common Cold Prodrome None One or more days Onset Sudden Gradual Fever 101 to 102 degrees F Rare in adults Headache May be severe Rare Myalgia Usual, often severe Mild Extreme exhaustion Usual Never Tiredness/weakness May last longer than two weeks Mild Sore throat Common Often Sneezing Occasionally Usual Rhinitis Occasionally Usual Cough Usual, nonproductive Mild hacking Which of the following influenza-type illnesses peaks in the winter?
Click to ReviewIt may be helpful to consider the time of year in which the diagnosis is being made. Generally, pneumococcal disease peaks in the winter, as does influenza and RSV. Mycoplasma and legionellosis are more common during the summer and fall. Rhinoviruses and parainfluenza virus peak during the fall and spring. Adenoviruses circulate throughout the year [21]. COVID-19 has had severe winter peaks but has been unpredictable thus far, with lesser peaks several times each year, corresponding with the emergence and spread of new variants [23]. Information on the presence of influenza and predominant strains in the community can usually be found from the surveillance system maintained by the local health department [11].
Influenza virus and acetylsalicylic acid interact to produce
Click to ReviewAn unfortunate complication of influenza in patients younger than 18 years of age is Reye syndrome. Much education for parents has focused on the danger of giving aspirin to anyone younger than 18 years of age with a fever. This education has led to a decrease in Reye syndrome. Unfortunately, acetylsalicylic acid or salicylic acid is a component in some over-the-counter preparations and may be unintentionally given to a child with a fever. Influenza virus, especially influenza A virus, and varicella (chicken pox) interact with acetylsalicylic acid to produce Reye syndrome. Symptoms are nausea and vomiting, decreased consciousness and/or convulsions caused by cerebral edema, hypoglycemia, and liver failure. Parents must be reminded to read the labels of all medications and that aspirin is listed as acetylsalicylic acid [16].
Influenza vaccine
Click to ReviewInfluenza vaccine is the primary preventive measure against the virus. It is efficacious in preventing influenza. Among those at higher risk, it lessens the severity of the illness, decreases complications, reduces hospitalizations, and lowers the fatality rate. It is disappointing that a vaccine with such benefits and few side effects is not used more widely. With a highly communicable disease like influenza, children are the most likely to contract and spread the infection. Nearly all children must be immune to achieve community (herd) immunity [32]. The Advisory Committee on Immunization Practices (ACIP) recommends routine annual influenza vaccination for all persons 6 months of age and older who do not have contraindications [11]. A licensed, recommended, and age-appropriate vaccine should be used.
Live attenuated influenza vaccine (LAIV) is
Click to ReviewLive attenuated influenza vaccines (LAIVs) have been in development in the United States since the 1960s [70,71]. FluMist (a LAIV trivalent formulation), manufactured by MedImmune, LLC, was originally approved in June 2003. FluMist trivalent LAIV contains two subtype A strains and two subtype B strains. It was approved by the FDA in February 2012 and was first available for the 2013–2014 flu season [61,72]. FluMist, which is delivered intranasally, is licensed only for healthy, nonpregnant persons 2 to 49 years of age. Live vaccines are unsuitable for healthcare workers who care for immunocompromised patients [11].
For two flu seasons, FluMist was not recommended based on data indicating inefficacy of the formulation. However, FluMist was reintroduced in the 2018–2019 season [11,73]. People with chronic health conditions should not be given the intranasal vaccine. The ACIP does not recommend the use of LAIV in immunosuppressed patients, and family members of close contacts of severely immunocompromised individuals are advised to avoid contact with them for at least seven days following vaccination [61]. LAIV can be administered at the same time with other vaccines, live and inactivated, but if not given at the same time, should be given four weeks after any other vaccine. In September 2024, FDA approved FluMist (LAIV3) for self-administration (for recipients 18 through 49 years of age) or administration by a caregiver ≥18 years of age (for children and adolescents 2 through 17 years of age). FluMist for self-administration or caregiver administration is anticipated to become available during the 2025–2026 season [11].
LAIV appears to induce both mucosal and serum antibodies. It is easier to administer than an IM injection, and it is preferred in some cases. In addition, no serious illnesses have been reported among unvaccinated contacts who were infected by those who had received the live vaccine [11].
A Healthy People 2030 objective is to
Click to ReviewThe Healthy People 2030 objective is to increase the proportion of persons who are vaccinated annually against seasonal influenza to at least 70% of the target population, but obviously 100% coverage is preferable [75]. To emphasize the importance of flu vaccinations, the CDC has established the National Influenza Vaccination Week. The first week of December 2025 has been designated national influenza vaccination week [76]. In the 2023–2024 flu season, vaccination coverage with one or more doses of flu vaccine was 55.4% among children 6 months through 17 years, a decrease of 2.0 percentage points compared with the 2022–2023 flu season (57.4%) and a decrease of 8.3 percentage points compared with the pre-pandemic 2019–2020 season (63.7%). The last time flu vaccination coverage among children was this low or lower was the 2011–2012 season (51.5%). Flu vaccination coverage among adults 18 years of age and older was 44.9%, a decrease of 2.0 percentage points from the prior season (46.9%). For adults, after an initial increase in flu vaccination coverage in the season immediately following the start of the COVID-19 pandemic, coverage has steadily declined since the 2020–2021 season. The last time flu vaccination coverage among adults was lower was during the 2017–2018 season (37.1%).[77].
The most effective way to increase the use of influenza vaccine is for
Click to ReviewOne of the major factors in increasing the number of administrations of influenza vaccine is the involvement of the medical practitioner providing care in a variety of settings, such as physicians' offices, clinics, outpatient rehabilitation programs, or any place where there is contact between medical providers and their patients. To encourage practitioner involvement, providers should be informed of the reimbursement for the vaccine and its administration by Medicare and Medicaid and should be instructed as to billing methods, especially roster billing.
The majority of flu shots given are administrated by the person's personal healthcare provider, and studies have shown that a healthcare provider's recommendation plays a critical role in a patient's decision to get a seasonal flu vaccine [83]. As many as 75% of patients at high risk for influenza or for death from a complication of influenza have seen a healthcare provider in the last year. One of the most effective methods of encouraging a high-risk patient to receive the flu shot is a verbal recommendation from the patient's physician [83].
Standing orders are
Click to ReviewImplementation of standing orders in acute care hospitals is another way to help increase influenza vaccine coverage. Patients who are hospitalized as flu season approaches, or during flu season, should have their records checked for chronic illness that is impacted by influenza and for influenza vaccine status. Those who have risk factors for complications and have not received the influenza immunization should receive the flu shot before discharge, as covered by the standing order. Such standing orders would have to be developed and implemented by the medical board of the hospital. All medical personnel connected with the hospital should be made aware of the standing order and reminded by posters or other means during influenza season. A study of Medicare patients hospitalized during flu season showed that only 31.6% had received the flu vaccine before admission, 1.9% during admission, and 10.6% after admission [70].
Effective handwashing
Click to ReviewGood handwashing is difficult to practice, is rarely known or taught, and is one of the single most effective ways to prevent transmission of many diseases, including influenza. Everyone knows to wash their hands before eating and after using the restroom. However, few do little more than remove obvious dirt. Good handwashing involves removing the skin oils where organisms can remain even when the hands look clean. A quick pass under the water faucet and fast dry with a towel removes visible dirt, but the oils and organisms remain.
To effectively remove the oils and organisms, the process should take at least 20 seconds (e.g., the amount of time that it takes to sing "Twinkle, Twinkle Little Star"). The hands should be soaped and rubbed vigorously for 15 seconds to create a good lather and to assure that all parts of each hand are soaped and rubbed well. Then the hands should be rinsed thoroughly and dried, preferably with a paper towel. The towel should be used to turn off the water and then properly thrown away. Such handwashing removes the oils that harbor the organisms, but 20 second s can seem like a long time in the busy life of a healthcare provider. If there is no visible dirt or contamination, a waterless hand sanitizer with at least 60% alcohol can be used between patients. However, nothing is as good as washing well with soap and water. Some mistakenly think that hot water must be used to kill the organisms. Water hot enough to kill organisms would be too hot to touch. Warm water mainly adds to comfort and hopefully encourages better washing technique. Careful attention to handwashing and cleansing may result in chapped skin, so medical professionals should find the proper lotions to care for their hands [87,88].
One way a person becomes infected with the influenza virus is by
Click to ReviewThe eyes, nose, and mouth are entryways for bacteria and viruses. Everyone tends to unconsciously touch their eyes, nose, and mouth when going about their activities. Because organisms are not visible and handwashing is often less than adequate, infection occurs. Though difficult, persons trying to prevent illness should make a conscious effort to avoid touching their face [89].
Cough etiquette is
Click to ReviewCovering a cough or sneeze is of primary importance however it is done [90]. Ideally, disposable paper tissues will be readily available during cold and flu season and used to cover the nose and mouth when coughing or sneezing. Patients and children should be instructed that, when this is not possible, they should cough or sneeze into their upper sleeve or elbow instead of into their hands. This will avoid contaminating the hands with an offending virus or bacteria [90]. In those instances when coughs and sneezes are covered with only the bare hands, the hands should be cleaned with soap and water or with an alcohol-based hand sanitizer as soon as possible to prevent transfer of the organisms to another person. Coughing, sneezing, or blowing nasal secretions into a cloth handkerchief is not recommended as this results in creating a moist, viable culture that is then carried in the pocket or purse, potentially resulting in prolonged episodes of re-infection or transfer from cross-contamination.
Which of the following antiviral medications are approved to treat influenza A and B?
Click to ReviewCOMPARISON OF ANTIVIRALS USED IN INFLUENZA
Characteristics Zanamivir Oseltamivir Peramivir Baloxavir Type of antiviral Neuraminidase inhibitor Neuraminidase inhibitor Neuraminidase inhibitor Endonuclease inhibitor Effective for type Influenza types A and B Influenza types A and B Influenza types A andBa Influenza type A and B, including avian strains and strains resistant to oseltamivir Route of administration Inhaled Oral IV Oral Age that can receive Treatment: 7 years of age and older Prevention: 5 years of age and older Treatment: 14 days of age and older Prevention: 1 year of age and older Treatment: 6 months of age and older Prevention: NA Treatment: 5 years of age and older Prevention: 5 years of age and older Action Decrease symptoms Decrease symptoms Decrease antibiotic use Decrease symptoms Decrease symptoms Side effects Throat/tonsil pain, nasal symptoms, diarrhea, nausea, headache, cough Nausea and vomiting Diarrhea Diarrhea, nasopharyngitis Sold as Relenza, Diskhaler Tamiflu Rapivab Xofluza aPeramivir efficacy is based on clinical trials in which the predominant influenza virus type was influenza A; a limited number of subjects infected with influenza B virus were enrolled. Amantadine was approved in 1966 as a treatment for uncomplicated respiratory tract illness caused by influenza. It belongs to a group of chemically related drugs called adamantanes (tricyclic amines) and is effective only against influenza A viruses. Rimantadine, approved in 1993, is also in the adamantanes group. Therefore, it is also only effective against influenza A. However, circulating influenza A (H3N2) and 2009 H1N1 viruses are resistant to adamantanes. As a result, these medications are no longer recommended for the treatment or prophylaxis of influenza A [61,94,103].
Any antiviral medication used to treat influenza should be started
Click to ReviewThe antiviral medications zanamivir and oseltamivir are also used to treat acute illness due to influenza (Table 3). To be effective, any of these medications must be started within 48 hours of symptom onset. Generally, a course of one of these antivirals will reduce the illness by one to two days, prevent serious complications, and make the patient less contagious to others. These medications are effective only against influenza viruses and will not affect the common cold or other ILI of viral origin [61,94,96]. All require a prescription from a physician.
Antiviral medications have been demonstrated to
Click to ReviewThe antiviral medications zanamivir and oseltamivir are also used to treat acute illness due to influenza (Table 3). To be effective, any of these medications must be started within 48 hours of symptom onset. Generally, a course of one of these antivirals will reduce the illness by one to two days, prevent serious complications, and make the patient less contagious to others. These medications are effective only against influenza viruses and will not affect the common cold or other ILI of viral origin [61,94,96]. All require a prescription from a physician.
Resistance has been documented to
Click to ReviewSince 2005, some resistance to all of the antivirals has been documented. However, the 2009 H1N1 outbreak remained sensitive to oseltamivir except in a few cases [11]. Serious reactions to the four antiviral medications should be reported to the FDA MedWatch program.
A point in the care of the patient with influenza is
Click to ReviewPoints in the care of the patient include: careful observation, providing symptomatic relief, help with activities of daily living, helping the patient remain hydrated, and emotional support (Appendix 1).
In caring for a high-risk patient during flu season, it is important to
Click to ReviewAttention should also be given to the person(s) caring for the patient with influenza in the home to protect him/her from the disease. This would include influenza immunization, with or without an antiviral medication for two weeks, instruction on effective handwashing, wearing a mask when providing care or when the patient is coughing, getting adequate rest, consuming five to nine or more fruits, fruit juices, and vegetables each day, and drinking eight glasses of water every day (Appendix 2).
Avian influenza is a special concern because
Click to ReviewWhenever an AI virus infects a human directly, there is much concern. Humans rarely have any immunity to AI viruses. Medical resources around the world quickly mobilize when there is a case of AI that skips reassortment in swine and directly infects a human. Fowl within a 2-mile (3-kilometer) radius of the source bird/flock are killed in order to contain the virus. An AI virus in humans usually produces upper respiratory disease and conjunctivitis. The infected humans and their contacts are watched closely for secondary transmission. For a pandemic to follow, these factors are needed:
Humans do not have immunity to the virus
Direct transmission from bird to human
Sustainable transmission from human to human
Movement of infected/contagious individuals to other geographic locations
What elements are needed for an avian influenza pandemic to occur?
Click to ReviewWhenever an AI virus infects a human directly, there is much concern. Humans rarely have any immunity to AI viruses. Medical resources around the world quickly mobilize when there is a case of AI that skips reassortment in swine and directly infects a human. Fowl within a 2-mile (3-kilometer) radius of the source bird/flock are killed in order to contain the virus. An AI virus in humans usually produces upper respiratory disease and conjunctivitis. The infected humans and their contacts are watched closely for secondary transmission. For a pandemic to follow, these factors are needed:
Humans do not have immunity to the virus
Direct transmission from bird to human
Sustainable transmission from human to human
Movement of infected/contagious individuals to other geographic locations
Swine influenza is usually caused by which virus subtype?
Click to ReviewSwine influenza is usually caused by the H1N1 subtype, but other swine influenza A viruses do occur, including H1N2, H3N1, and H3N2 [149]. Although swine flu viruses do not normally infect humans, sporadic human infections have occurred. When this occurs, these viruses are called "variant viruses" and are denoted by adding the letter "v" to the virus subtype designation. Human infections with H1N1v, H3N2v, and H1N2v viruses have been detected in the United States [149]. Pigs may become infected with more than one virus subtype simultaneously; in these cases, genes from the viruses may mix and create a new "reassortment" virus [150]. The main swine influenza viruses circulating in U.S. pigs in the past decade include triple reassortant (tr) H1N1, trH3N2, and trH1N2 [151].
- Back to Course Home
- Participation Instructions
- Review the course material online or in print.
- Complete the course evaluation.
- Review your Transcript to view and print your Certificate of Completion. Your date of completion will be the date (Pacific Time) the course was electronically submitted for credit, with no exceptions. Partial credit is not available.